Understanding Low Back Pain
Pain Management Toolkit
Low Back Pain (LBP)
Commonly defined as pain and discomfort that is localized to the posterior region of the lower ribs and upper thighs +/- leg pain.
- There are many classifications of LBP:
- Mechanical (non-specific) low back pain
- Disc-related low back pain
- Spinal stenosis (arthritic changes)
- Other structural & degenerative changes
Identify the movements, postures or activities that are aggravating your back pain. By recognizing the causes of irritation we can stop “picking at the scar” and allow healing to take place.
It’s never, “I have to stop”,
it’s always, “I have to modify”.
Pain Management Toolkit
- Understand your pain
- Posture & movement retraining
- Stay active (in your own way)
- Setbacks are OK
- Consistency and patience
Understand Your Pain
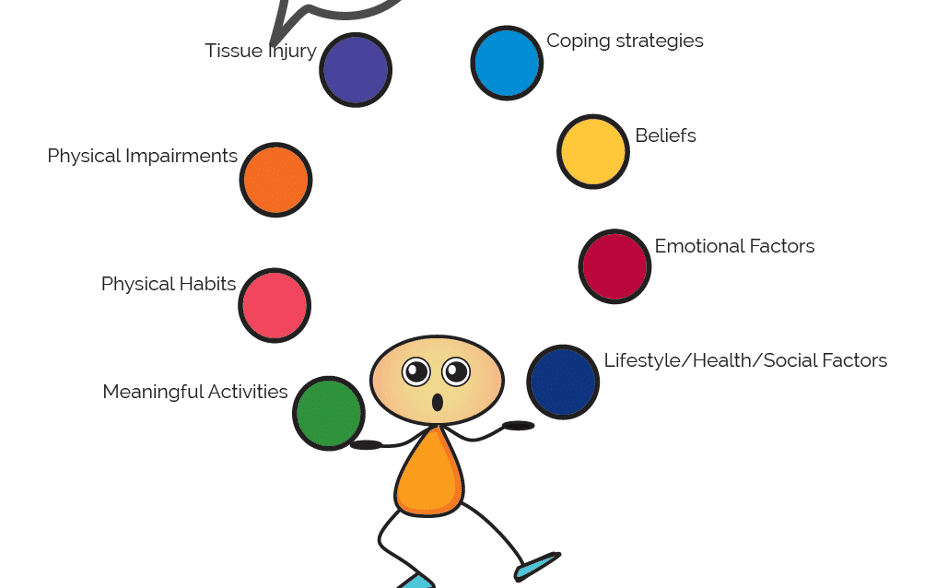
There are many factors that contribute to the experience of LBP and each component is as important as the next to address in recovery. Pain isn’t always a sign of tissue damage or injury. For instance, fears related to the injury, different life stressors or the spontaneous firing of nerves without any stimulation can result in the experience of pain. Below are various different factors that impact pain.
Biological: pain sensitized tissues (muscles, nerves, tendons, ligaments, joints)
Emotional: frustration, fear, anxiety, stress, etc.
Social: restriction or withdrawal from activities we enjoy, and the people associated with such.
Cognitive: thoughts and beliefs about your pain.
Posture & Movement retraining
The sensations we experience – pain, spasms, shooting, sharpness, aches – is often a result of the body not feeling safe with the movement. It’s all about teaching the body that it’s safe to move. When getting past LBP, it is important to identify movements and activities that feel good vs. those that exacerbate your pain.
- Figure out which movements and postures you are sensitive to (e.g. bending, twisting, prolonged postures such as sitting, standing, crouching)
- Calm down the sensitivity
- Gradually build up resiliency, strength, confidence, and adaptability.
 Stay active (in your own way)
Stay active (in your own way)
There is no evidence available to show that one type of exercise is superior to another. In deciding on the type of exercise to be used, guidelines should, however, incorporate individual preferences, needs, and capabilities…
– Shipton, E.A. Physical therapy approaches in the treatment of low back pain. Pain Ther. 2018, 7, 127-137.
You may have heard core and hip exercises are a great option – and they are! However, it’s important to find what works best for you and continue to modify activities to listen and respect your pain levels. Research indicates that there is no evidence to showing one exercise is better than the other, rather it suggests that a diversity of types of exercises should be used. The best exercise is based on what your body needs and what it is able to do.
The purpose of exercises isn’t to “stabilize your spine”, improve your flexibility or to build rock-hard abs, rather it is to gradually teach the body it is safe to move – “motion is lotion”. As we begin to move more and more, this allows us to gradually build up our resiliency, strength and confidence.
Below are some ideas for staying active:
- Walk
- Yoga
- Stretch
- Hydrotherapy
- Swimming
- Tai Chi
- Isometric Exercises
- Core exercises
- Group classes
- Weight training
- Foam rolling
- Biking
- Elliptical
- X-country skiing
- Hiking
Setbacks are ok (and very normal)
Studies indicate that, “Recurrence of low back pain is very common, with more than two-thirds (~66.6%) of individuals having a recurrence within 12 months after recovery.
T. da Silva, K. Mills, B.T. Brown, N. Pocovi, T. de Campos, C. Maher, M.K. HancockRecurrence of low back pain is common: a prospective inception cohort study J Physiother, 65 (2019), pp. 159-165
Think of recovery as an upward trend – there will be ups and downs along the journey, but overall, you’re headed in the right direction and will not fall back to the lowest point.
Up to two-thirds of individuals with low back pain will experience a re-aggravation of their back within 12 months. Therefore, a repeat episode of low back pain doesn’t mean you’ve failed rehab or that what you’re doing isn’t working. It’s just a time for you to implement different tools from your toolkit and proactively manage the pain before it increases.
The goal isn’t to eliminate or stop doing things that are important to you, but to modify along the way.
Consistency and Patience
Full recovery timelines depend on the type of injury; however, most episodes of low back pain will begin to improve within 6-8 weeks. Despite bumps along the way, if you “focus on the process and trust in the hard work” [quoting Kobe], things will improve.
How does physiotherapy help?
Physiotherapy can help you by providing guidelines on different types of exercises and activities, providing education on different topics related to low back pain (e.g. pain science, recovery timelines, latest research direction, sleep positions), using manual therapy techniques to temporary manage pain, movement examination and modifications, as well as referring to other healthcare providers as needed for other medical interventions.
Bottom line: Pain is not just about damage, meaning you have lots of options to treat your pain.
– Greg Lehman
“Prevention and treatment interventions having an exercise component are most likely to be effective”
Michaleff ZA, Kamper SJ, Maher CG, Evans R, Broderick C, Henschke N. Low back pain in children and adolescents: a systematic review and meta-analysis evaluating the effectiveness of conservative interventions. Eur Spine J. 2014;23:2046–2058. doi: 10.1007/s00586-014-3461-1.


